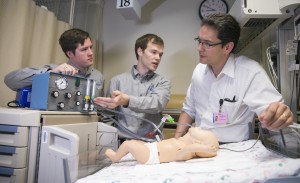
What started off as a mandatory capstone project to help BYU engineering students graduate has turned into a life-saving device that could help thousands of prematurely born infants around the world.
“The World Health Organization reports that newborn asphyxia (the inability to breath regularly at birth) is one of the leading causes of infant mortality in developing countries,” said Jim Trent, external relations manager for BYU’s Department of Mechanical Engineering, “accounting for 4 to 9 million deaths annually, or about twenty percent of the infant mortality rate.”
Recent BYU graduate Spencer Ferguson, along with several other classmates, has developed a new ventilator system called the NeoLife ventilator, that will be more cost effective for many Third World countries. With ordinary ventilator machines in newborn intensive care units costing upward of $40,000, the newly designed machine was developed for about 98.75 percent less than that cost.
“The students were able to get (the unit) down to about $500,” Trent said.
While the current prototype may not have all of the bells and whistles of the more sophisticated ventilator models, “any function you need to keep the patient alive, it has that,” said Ferguson, team leader for the second-year group that developed the product.
With the environment of many Third World medical clinics being unpredictable, the product is built to last.
“All the main components will last two years,” Trent said.
The project was first developed after Utah Valley Neonatologist Erick Gerday and his colleagues came back from neonatal resuscitation training in Third World countries having witnessed firsthand the heartbreak of parents losing their babies because they have to manually ventilate the premature baby by hand, a practice known as “bagging.”
“It’s pretty heartbreaking to watch,” Trent said. “If (the ventilators) go too slow the baby can have brain damage; if they go too fast the little lung can pop. It’s hard to keep going.”
Ferguson mentioned that the pump requires frequent attention; leaving it for too long could be fatal.
“Every two seconds they have to pump. If they fall asleep, the baby dies,” he said.
“The doctors were falling over themselves with excitement because this is what they envisioned,” Trent said after the project was finished and showed to Gerday and his colleagues.

The project was sponsored by local philanthropist John Krupa. Krupa was originally planning on serving a LDS mission with his wife but, due to medical reasons, was unable to. Instead, he used the money he would have used to fund his mission to pay for the $20,000 sponsorship fee required for the capstone project.
The project was originally started in fall of 2013 and has taken two years to develop, with students working a minimum of two hours per day for four consecutive semesters. A total of two teams, 12 students, several professors and two neonatologists contributed to the current prototype.
“Last year they started with nothing and ended up with a working prototype which wasn’t anywhere near ready to be used. We started testing it and trouble shooting. We took it from where it was and got it ready for testing, as well as being able to be mass produced,” Ferguson said.
When asked if the current prototype is ready to be mass produced, Trent said that “other than animal testing, it’s really close.”
Before the product can be shipped out and donated to Third World countries like the Philippines and several nations in Africa, it has to go through extensive testing for three days. Luckily for Ferguson and his team they don’t have to travel very far to test their machine.
“The University of Utah has one of the world-leading premier labs for exactly what we’re doing, neonatal ventilation studies,” Ferguson said.
Unlike the machine the students have created, the testing comes with an expensive price tag.
“Our biggest challenge now is raising funding to pay for that testing. We need about $25,000–$30,000,” Ferguson said.
Krupa, the team’s sponsor, has already received interest from several nonprofit organizations, including the Bill & Melinda Gates Foundation and LDS Charities, to fund the production of thousands of units to be donated to countries in need.
When asked what their timetable was to raise the necessary funding for testing, Trent answered without hesitation, “Yesterday … but honestly, within the next few months we’d like to move forward,” he said.
Ferguson voiced a similar frustration, saying, “We have a device that can save hundreds of thousands of lives, and it’s just sitting here, doing nothing.”
The team has set up a website for donations. Currently the engineers have $720 of their goal of $25,000.




