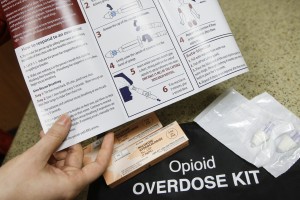
The overdose reversal drug Naloxone has become a hot topic in a state with skyrocketing opioid overdose death rates.
Some supporters of the drug work in health care. Some are loved ones of overdose victims. Derek Nelson is both.
Nelson, a nurse who works for Emergent Biosolutions, lost his stepson, Hayden, to an opioid overdose in June. Hayden had only been home from a 34-day treatment program for five days when he died.
“I look at it now and just shake my head thinking how crazy it is that, even when we went to pick up Hayden after these emergency room and acute detox situations, somebody didn’t hand over Naloxone at that point and just say, ‘Here, in case you get into trouble,’” Nelson said.
Reps. Carol Spackman Moss, D-Salt Lake City, Mike McKell, R-Spanish Fork, and Steve Eliason, R-Sandy, have drafted bills this legislative session under the umbrella of an opioid overdose response act. The bills have all moved through the Health and Human Services Committee with favorable recommendations and are now up for debate in the House.
Spackman Moss said Utah ranks fourth in the nation for prescription drug overdose deaths and first for prescription drug overdose deaths among veterans. HCR4, which passed the committee unanimously, declared the situation a public health emergency.
The bills address different facets of a larger program that would increase availability of Naloxone, a drug that can temporarily reverse the effects of an opiate overdose. Naloxone can be administered through a syringe or through a nasal spray and has no harmful side effects.
Eliason’s bill, HB240, would issue a standing order for all healthcare providers to prescribe Naloxone in tandem with regular opiate prescriptions.
Eliason was introduced to the issue by one of his constituents, a father whose son died of a heroin overdose. Eliason said he is most proud of bills brought before him by Utahns.
McKell’s HB192 authorizes a pilot program that would grant money, particularly to rural counties, to get Naloxone into the right hands. It would dispense the drug to law enforcement divisions, schools and organizations for the homeless.
Some of these groups have been hesitant to use Naloxone for fear of liabilities. McKell is also sponsoring HB239, which ensures that someone who used the reversal agent “in good faith” on an overdose victim would be protected from legal punishment if anything went wrong.
McKell believes funding is the key to lowering Utah’s opiate overdose death rates.
“I’m asking for a significant chunk of money to put money on the ground and really make a difference,” McKell said.
Randle Likes, chief medical officer at Timpanogos Hospital in Orem, said his main concern about treatment with Naloxone away from a hospital is the behavior of the recipient when they wake up. In his experience, opiate addicts become “combatant and aggressive” when they regain consciousness.
“If you’ve got people like that at home that are getting some Naloxone, it wakes them up, and then they get mad at whoever gave it to them … they are almost certainly going to relapse,” Likes said.
Spackman Moss’s bill, HB238, addresses Likes’ worries. The bill would allow outreach provider groups, not just pharmacists and physicians, to dispense Naloxone. It provides for education on administering Naloxone, and the crucial first step in the instructions is to call 911.
Likes thinks the bills are good ideas, but says they’re avoiding the real problem.
“I think healthcare providers are concerned that the overall problem is really what needs to be addressed and not just these little Band-Aid fixes,” Likes said.
Brian Allen, representing the pharmaceutical workers compensation company Helios, speaks and lobbies nationwide on the opiate epidemic. He testified at a recent committee hearing, saying, “We have to change the prescribing culture in our country.”
Nelson learned of a friend who, after an elbow surgery, received a prescription for 100 Oxycontin pills. He used three.
Nelson thinks other parts of the root problem include insufficient treatment programs and flawed public perception of substance abuse.
“If we had the same number of people being killed by HIV or the new Zika flu, everybody would be outraged,” Nelson said. “But we view substance use disorders as, for whatever reason, something that we’re willing to live with and not talk about.”
And the committee agreed. Openly admitting that Naloxone is a Band-Aid fix, Eliason gave an analogy to explain the reasoning behind the bills.
“Nobody thinks a fire is a good thing, and all the talk generally is about fire prevention. However, when a fire starts, you need an extinguisher,” Eliason said. “You need to have a last resort to save people’s lives.”
Dr. Jennifer Plumb, a pediatric emergency specialist at Primary Children’s Medical Center, worked together with her brother to found Utah Naloxone. The program dispenses and teaches people how to use Naloxone. She said 22 overdose reversals have been reported to Utah Naloxone in the past six months.
“It’s something that can help in the short term, and I hope it’s something that drives a better conversation for the long term,” Nelson said.




